Managing patient records the old way is costly. Missing files, delayed updates, and data errors put both patients and providers at risk. That’s where Electronic Health Record (EHR) systems come in.
An EHR system is a digital platform that stores, manages, and shares patient health data in real time. It keeps everything from diagnoses to prescriptions in one place.
But building one isn’t as simple as it sounds. From choosing the right features to staying compliant with healthcare regulations, there’s a lot to get right.
This post breaks down everything about EHR system development.
What is EHR Software?
EHR software, or Electronic Health Record software, is a digital system that stores and manages patient health information. It replaces paper-based records with a structured, easy-to-access format.
Healthcare providers use it to record patient visits, track medical history, manage prescriptions, and share data across departments. It keeps everything in one place, organized and up to date.
Unlike basic record-keeping tools, EHR software connects different parts of a healthcare system. Doctors, nurses, and admin staff can all access the same data in real time.
Simply put, it’s the digital backbone of modern healthcare management.
Key Benefits of EHR Software Development
Building EHR software brings real, measurable changes to how healthcare works. Here are the key benefits worth knowing about.
- Faster Access to Patient Data: Healthcare teams can pull up patient records instantly. No more waiting or searching through physical files.
- Fewer Medical Errors: Digital records reduce the chances of miscommunication. Accurate data means safer treatment decisions.
- Better Care Coordination: Different departments can share patient information easily. This keeps everyone on the same page.
- Lower Operational Costs: Going digital cuts down on paperwork and admin work. It saves both time and money over the long run.
- Stronger Data Security: EHR systems store sensitive data with encryption and access controls. Patient information stays protected at all times.
- Easier Regulatory Compliance: Built-in tools help healthcare providers meet data and privacy laws. Staying compliant becomes much less of a hassle.
- Improved Patient Experience: Patients get faster service and fewer repeat tests. Their care feels more personal and well-informed.
Many of these advantages align with findings shared by HealthIT.gov on how EHR systems improve healthcare outcomes.
Essential Features of a Modern EHR System
A well-built EHR system comes packed with features that make healthcare management smoother and more reliable. Here’s what matters most.
1. Patient Data Management
At its core, EHR software stores complete patient profiles: medical history, allergies, diagnoses, and more. All data stays updated in real time, making it easy for any authorized provider to access accurate information during a consultation.
2. Clinical Documentation
Doctors and nurses can record visit notes, treatment plans, and observations directly into the system. This removes the need for paper-based documentation and keeps clinical records clean, consistent, and easy to retrieve later.
3. Appointment Scheduling
The system lets staff book, reschedule, and track patient appointments from one dashboard. Automated reminders reduce no-shows, and the scheduling tool syncs with provider availability to avoid conflicts or double bookings.
4. E-Prescribing
Providers can send prescriptions directly to pharmacies through the EHR platform. This cuts out handwritten prescriptions, reduces errors, and speeds up the process for both the patient and the pharmacy team.
5. Lab and Test Integration
EHR systems connect with diagnostic labs to pull in test results automatically. Providers can view reports without delay, which helps them make quicker and more informed treatment decisions for their patients.
6. Billing and Coding Support
The software links clinical data with billing processes. It auto-generates medical codes based on recorded diagnoses, which reduces manual entry errors and makes insurance claims faster and more accurate to process.
7. Interoperability
A strong EHR system shares data across different hospitals, clinics, and health platforms without friction. This means patient records follow them wherever they go, giving every provider a full picture of their health.
8. Patient Portal
Patients get their own secure login to view records, test results, and upcoming appointments. This gives them more control over their health and builds stronger communication between patients and their care providers.
Step-by-Step EHR Software Development Process
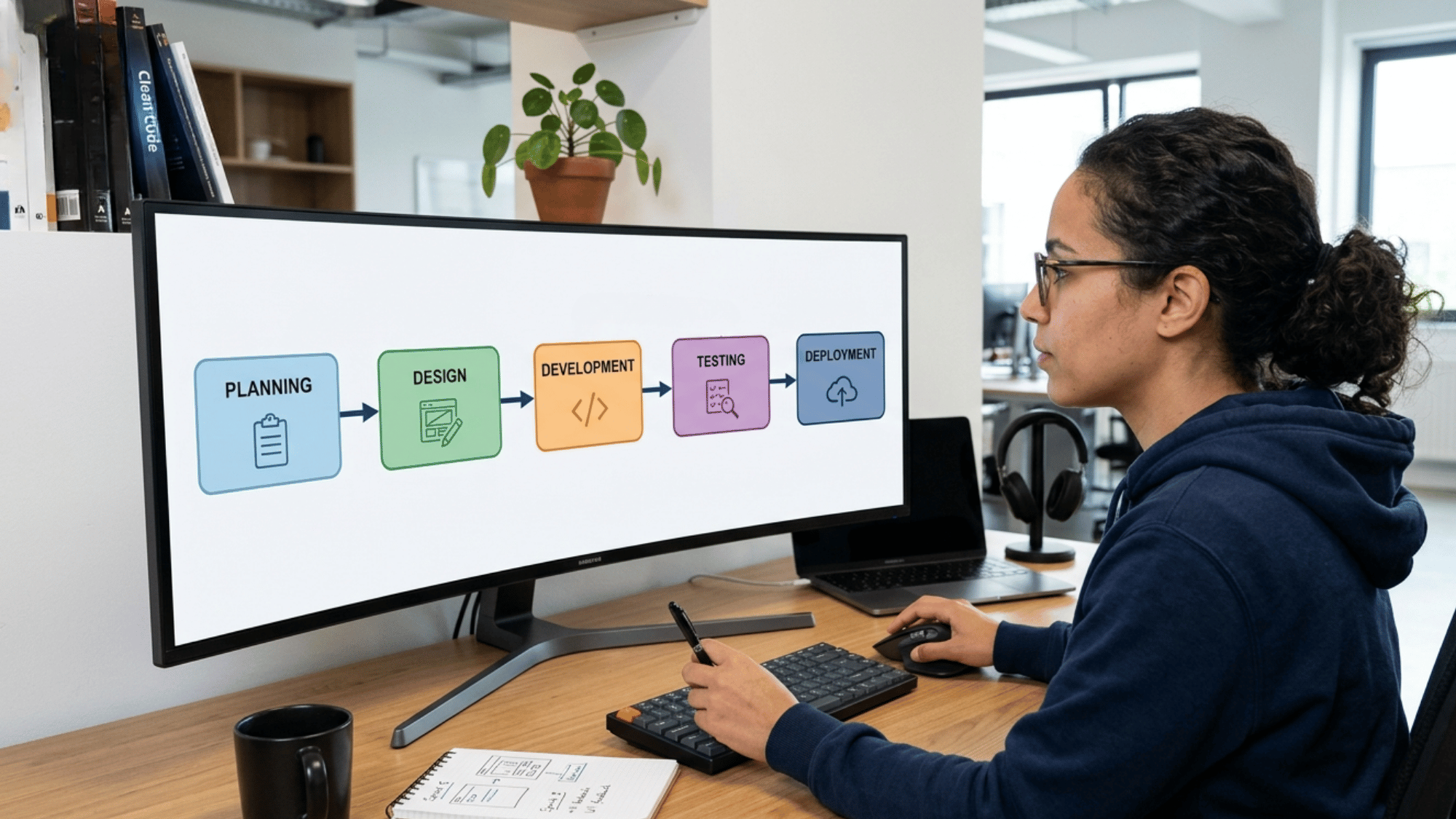
Building EHR software takes careful planning and execution. Here’s a clear breakdown of each step in the development process.
Step 1: Define Goals and Requirements
Every solid EHR project starts with a clear plan.
Development teams work with healthcare providers to understand what the system needs to do. This includes identifying the target users, core features, compliance needs, and workflow gaps.
Getting this step right saves a lot of time and rework later in the process.
Step 2: Assemble the Right Development Team
EHR development needs more than just good coders.
The team should include software developers, UI/UX designers, healthcare consultants, compliance experts, and QA testers. Each role brings something critical to the table.
A well-rounded team makes sure the final product works well both technically and within real healthcare settings.
Step 3: Choose the Right Tech Stack
Picking the right tools and technologies shapes how the software performs. The team selects a programming language, database system, cloud infrastructure, and security frameworks based on the project’s scope.
The tech stack also needs to support future updates and integrations with third-party systems like labs and pharmacy networks.
Step 4: Focus on UI/UX Design
Healthcare professionals are busy. The interface needs to be clean, simple, and fast to use.
Designers create wireframes and prototypes based on real user workflows.
Good UX design reduces training time, lowers the chance of input errors, and makes daily tasks feel less overwhelming for doctors, nurses, and admin staff.
Step 5: Develop and Integrate Core Features
This is where the actual building happens. Developers code the core modules: patient records, scheduling, billing, e-prescribing, and more.
Each feature gets built and tested in stages. The team also works on integrations with external systems like diagnostic labs, insurance platforms, and other hospital management tools already in use.
Step 6: Test for Performance and Compliance
Before launch, the software goes through thorough testing. This includes functional testing, load testing, and security audits.
Compliance checks make sure the system meets healthcare data regulations like HIPAA. Any bugs or gaps found during this phase get fixed before the product moves forward to deployment.
Step 7: Deploy, Train, and Maintain
Once testing is complete, the software gets deployed in a live environment.
Staff training sessions help users get comfortable with the system quickly. Post-launch, the development team monitors performance, rolls out updates, and fixes any issues that come up.
Ongoing maintenance keeps the software running smoothly over time.
EHR Software Development Cost Breakdown
Building an EHR system is a significant investment. The total cost depends on several factors: the size of the project, the features needed, the development team’s location, and the technology used.
A basic EHR system with core features costs less than a fully custom-built platform loaded with advanced tools.
Ongoing costs like hosting, maintenance, and compliance updates add to the overall budget too.
There’s no one-size-fits-all number here. Every healthcare organisation has different needs, and the cost reflects that. Understanding what drives the price helps in making smarter budget decisions from the start.
Disclaimer: Cost figures vary based on project scope, team location, and technology choices. Consult a development partner for accurate estimates.
EHR Compliance & Regulatory Requirements
EHR systems handle sensitive patient data. Meeting compliance and regulatory standards is not optional; it’s a core part of development.
- HIPAA (Health Insurance Portability and Accountability Act): This is the primary data privacy law in the US. EHR systems must protect patient information through strict access controls, encryption, and audit trails.
- HL7 and FHIR Standards: These frameworks define how health data gets shared between systems. EHR software must support these standards to exchange information smoothly across different healthcare platforms and providers.
- ONC Certification: In the US, EHR systems used by healthcare providers need certification from the Office of the National Coordinator for Health IT. This confirms the software meets federal interoperability and functionality requirements.
- GDPR (General Data Protection Regulation): For EHR systems used in Europe, GDPR sets strict rules on how patient data gets collected, stored, and processed. Non-compliance can result in heavy financial penalties.
- 21st Century Cures Act: This US regulation focuses on stopping information blocking. EHR systems must allow patients and providers to access and share health data freely without unnecessary restrictions.
- SOC 2 Compliance: This standard checks whether a software system manages data securely and responsibly. It covers five key areas: security, availability, processing integrity, confidentiality, and privacy.
- State-Level Regulations: Beyond federal laws, many states have their own healthcare data rules. Development teams must account for these local requirements depending on where the EHR system gets deployed and used.
Best Practices for Successful EHR Development

Following the right practices from the start makes EHR development smoother, safer, and more cost-effective. This is a quick look at what works best.
| Best Practice | Why It Matters |
|---|---|
| Involve end users early | Real feedback from doctors and nurses shapes a more usable system |
| Prioritise data security from day one | Building security in later costs more and leaves gaps |
| Plan for scalability | The system should handle growth without major rebuilds |
| Follow compliance standards throughout | Fixing compliance issues post-launch is expensive and risky |
| Test early and test often | Catching bugs in early stages saves significant time and money |
| Keep the UI simple | A clean interface reduces training time and daily user errors |
| Document everything | Clear documentation helps with future updates and team onboarding |
| Choose interoperable technologies | Systems that connect easily with others deliver far more value |
Challenges in EHR Software Development
EHR development comes with its fair share of roadblocks. Here are the most common challenges development teams run into.
- Getting different systems to share data without errors is still one of the biggest technical problems in EHR development.
- Healthcare data is highly sensitive, making it a constant target for cyberattacks and data breaches.
- Meeting ever-changing compliance rules across different regions adds layers of complexity to the development process.
- Migrating existing patient records from legacy systems to a new EHR platform without data loss is a tricky and time-consuming task.
- Building software that works well for doctors, nurses, and admin staff, all at once requires careful and repeated user testing.
- Keeping the system running without downtime in a live healthcare environment puts heavy demands on the infrastructure.
- Training staff to use a new system while they manage their regular workload slows down adoption and increases resistance to change.
- Scaling the software to handle growing patient volumes and new features without affecting performance takes significant planning from day one.
Future Trends in EHR Software Development
EHR software is not staying still. As technology moves forward, the way healthcare systems store, share, and use patient data is changing fast.
Artificial intelligence, better data sharing, and patient-first design are pushing EHR development in a new direction.
Healthcare providers are looking for systems that do more than just store records, they want tools that actively support better clinical decisions.
The demand for smarter, faster, and more connected EHR platforms is growing. Development teams that keep up with these shifts will build software that stays relevant and useful for years to come.
Conclusion
EHR software development is a big step, but it’s one that pays off. The right system cuts down on errors, keeps data secure, and makes life easier for everyone in a healthcare setting from doctors to admin staff.
Getting it right takes planning. The features, the compliance requirements, the development process every piece matters.
Healthcare providers who invest in a well-built EHR system today are setting themselves up for smoother operations tomorrow.
Got questions about EHR development or need help figuring out where to start? Drop them in the comments below, happy to help point things in the right direction.
Frequently Asked Questions
What are the Top 3 EHR Systems?
Epic, Oracle Health, and Meditech rank among the most widely used EHR systems across hospitals and healthcare networks globally.
What is the Easiest EHR to Use?
DrChrono and Practice Fusion are often praised for their clean interfaces and short learning curves among healthcare professionals.
What is the World’s Largest EHR Implementation?
The US Department of Veterans Affairs runs one of the largest EHR implementations worldwide, serving millions of patients across hundreds of facilities.
Who Created the First EHR?
Dr. Lawrence Weed introduced the problem-oriented medical record concept in the 1960s, laying the groundwork for modern EHR systems.